 :max_bytes(150000):strip_icc()/carbon_monoxide_poisoning_symptoms-5ae1f5763128340037c64a67.png)
This makes the symptoms are subtle, if noticeable at all. It does not pose as immediate a risk as acute respiratory acidosis, and, because it happens little by little, the body adapts to the blood's acidity. This is a condition known as acute respiratory acidosis, and it is is a life-threatening medical emergency.Ī less severe form of respiratory acidosis, known as chronic respiratory acidosis, can happen gradually over time. Respiratory failure happens when you have so much CO2 in your blood that it raises your blood's acidity beyond healthy levels. 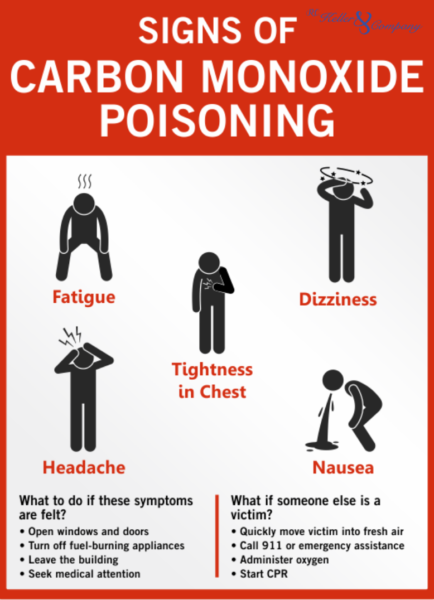
If it gets too bad, severe hypercapnea can cause respiratory failure, organ damage, and death. Left unchecked for too long, CO2 retention deprives your body of oxygen, which can cause serious health problems like heart disease, pulmonary hypertension, and cognitive dysfunction. That's why it's important to understand what CO2 retention is, how it happens, and how to recognize it the sooner you realize it's happening, the sooner you can seek treatment and get your COPD back under control. 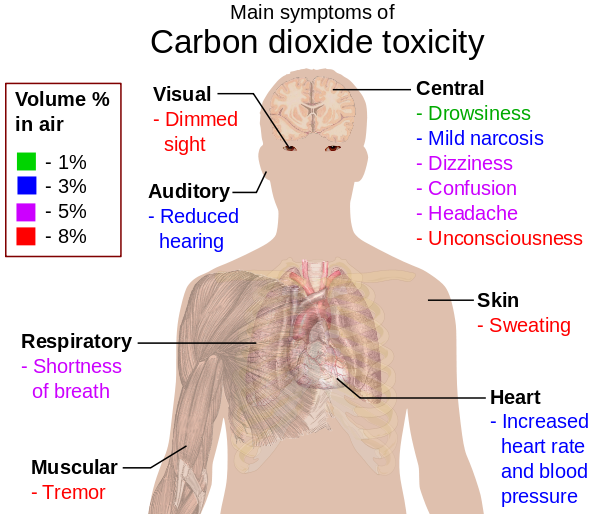
In fact, the early symptoms of CO2 retention may be so mild or non-existent that you don't notice them until it gets much worse. You are more likely to experience hypercapnea during symptom flare-ups, respiratory illnesses, and COPD exacerbations, but CO2 retention can also happen slowly and gradually over time. However, CO2 retention poses a more immediate risk of making your COPD more difficult to manage and making symptoms like coughing, wheezing, and shortness of breath worse. If left untreated for too long, hypercapnea-related hypoxemia can cause serious health complications, including respiratory failure and death. When mild, this can often be corrected with supplemental oxygen therapy and other COPD medications, however, it can be caused by improperly-dosed oxygen therapy, as well.īecause of this, the main symptoms of hypercapnea overlap with the symptoms caused by hypoxemia, which happens when your blood oxygen saturation gets too low. The result is low blood oxygen levels (hypoxemia) and high blood carbon dioxide levels (hypercapnea) that make it more and more difficult to breathe. That causes this blood flow strategy in the lungs to break down less blood flows to the parts of the lungs that function efficiently, and more blood flows through damaged alveoli that are less capable (or completely incapable) of exchanging oxygen and carbon dioxide efficiently. However, this ventilation-perfusion ratio can get thrown off, usually because of high-flow oxygen therapy, COPD exacerbations, or other COPD symptoms. At the same time, they increase blood flow to the most healthy alveoli so they can absorb as much oxygen (and release as much carbon dioxide) as possible. Usually, your lungs constrict your blood vessels in such a way that they decrease the amount of blood that flows to poorly functioning air sacs that have been damaged by COPD. This happens when your body gets confused about which parts of your lungs to prioritize, which reduces the efficiency of gas exchange in your lungs. As that excess CO2 builds up in your blood, it causes an imbalance between your blood oxygen and carbon dioxide levels, which can cause serious symptoms and oxygen deprivation.Ĭo2 retention also happens through a phenomenon known as ventilation-perfusion mismatch. Over time, as your COPD progresses and your lung function declines, you may retain more and more carbon dioxide as you breathe. 
When you have COPD, there are fewer healthy alveoli and fewer places for this exchange to happen, which makes it difficult to get enough oxygen into your blood and also difficult to get enough CO2 out of your blood and into your lungs. This leaves excess CO2 trapped in your lungs after you exhale, which takes up space that is needed to hold oxygen-rich air when you breathe in.ĬOPD also damages and destroys your air sacs, or alveoli, which is where oxygen and carbon dioxide is passed between your blood and the air in your lungs. It does this in two ways: by destroying the tiny air sacs in your lungs, and by preventing you from pushing all of the air out of your lungs when you exhale.ĬOPD can make it difficult to breathe out because of airway narrowing, blockage, and other changes in the lungs. COPD can disrupt the process described above by preventing you from getting rid of enough carbon dioxide when you breathe. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
